
Emergency Department and Risk for Physical Restraint Study
We seek to examine a dataset that contains detailed data from all YNHH emergency room visits from 2013-2025 (~6 million cases). In addition, we have and are now in the process of cleaning a new dataset comprising all measures collected over the last 2 years of YNHH intensive outpatient clinics, which can be married to the ER data set to examine the relationship between treatment progress and trajectories and prior (and ultimately subsequent) emergency service use.
Individuals with mental illness are significantly more likely to experience physical health problems [1-6], and premature mortality [7-11].
Commonly reported concerns include chest pain, financial burden, and stigma [12-14]
Individuals with mental illness disproportionately seek care in the ED [15-19].
ED is a high-risk environment for practice, often grappling with high-demand and insufficient resources [20-22].
Doctors further lack established relationships with patients, making integration of potentially relevant background impractical if not impossible at times. [23]
Stigmatized attitudes towards those with MH can compromise both care and decision making [24, 25], particularly in the ED leading to misattribution of symptoms [26]
Patients describe stigma both specific to mental health and more generally (Isbel, 2025). ER carers describe challenges including which are magnified by the current system (fiscal and structural issues which reinforce negative attitudes) (Isbel, 2023). In a study conducted by Schick et al., 36% of EM providers felt unqualified to handle psychiatric emergency, and 80% reported negative interactions with psychiatrist (rejection of patients).
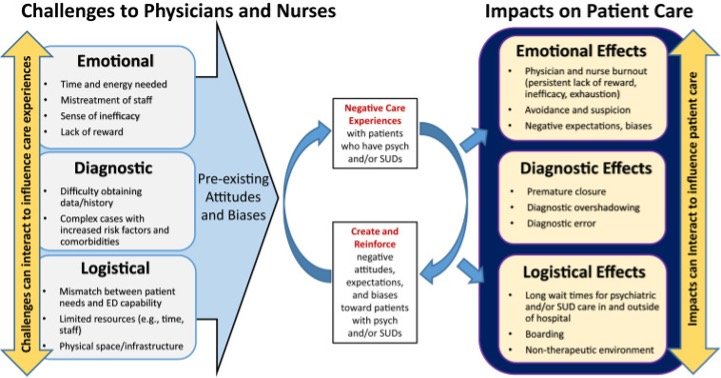
Figure citation: Isbell, L. M., Chimowitz, H., Huff, N. R., Liu, G., Kimball, E., & Boudreaux, E. (2023). A Qualitative Study of Emergency Physicians' and Nurses' Experiences Caring for Patients With Psychiatric Conditions and/or Substance Use Disorders. Annals of emergency medicine, 81(6), 715–727. https://doi.org/10.1016/j.annemergmed.2022.10.014
There are several aims for this project. We hope to examine differences in those who did and did not receive a psychiatric evaluation in the ER as they relate to demographics, presenting issue, language used in medical charts, number of repeat visits, and with high risk/stigmatized populations including individuals presenting with suicide behavior, a diagnosed personality disorder, or following a traumatic event. We also hope to examine differences in patients with and without mental health diagnoses, including information regarding likelihood of referral to mental health services, length of wait in ER and length/type of language used by medical providers, and number of repeated visits. Finally, we hope to examine patient change over time and the percentage of patients referred for psychiatric ER visits, the types of patients referred for psychiatric ER visits, and percentage of patients with mental health that received referral to services.
Suggested reading:
Citations:
1. M. De Hert, C. U. Correll, J. Bobes, et al., “Physical Illness in Patients With Severe Mental Disorders. I. Prevalence, Impact of Medications and Disparities in Health Care,” World Psychiatry 10, no. 1 (2011): 52–77, https://doi.org/10.1002/j.2051-5545.2011.tb00014.x.
2. G. M. Goodwin, “Depression and Associated Physical Diseases and Symptoms,” Dialogues in Clinical Neuroscience 8, no. 2 (2006): 259–265, https://doi.org/10.31887/DCNS.2006.8.2/mgoodwin.
3. M. C. Harter, K. P. Conway, and K. R. Merikangas, “Associations Between Anxiety Disorders and Physical Illness,” European Archives of Psychiatry and Clinical Neuroscience 253, no. 6 (2003): 313–320, https:// doi.org/10.1007/s00406-003-0449-y.
4. B. G. Druss, “Mental Disorders and Use of Cardiovascular Procedures After Myocardial Infarction,” Journal of the American Medical Association 283, no. 4 (2000): 506, https://doi.org/10.1001/jama.283.4.506.
5. G. Sullivan, X. Han, S. Moore, and K. Kotrla, “Disparities in Hospitalization for Diabetes Among Persons With and Without Co-Occurring Mental Disorders,” Psychiatric Services 57, no. 8 (2006): 1126–1131, https://doi.org/10.1176/ps.2006.57.8.1126.
6. E. E. McGinty, J. Baller, S. T. Azrin, D. Juliano-Bult, and G. L. Daumit, “Quality of Medical Care for Persons With Serious Mental Illness: A Comprehensive Review,” Schizophrenia Research 165, no. 2–3 (2015): 227–235, https://doi.org/10.1016/j.schres.2015.04.010.
7. J. F. Hayes, J. Miles, K. Walters, M. King, and D. P. J. Osborn, “A Systematic Review and Meta-Analysis of Premature Mortality in Bipolar Affective Disorder,” Acta Psychiatrica Scandinavica 131, no. 6 (2015): 417–425, https://doi.org/10.1111/acps.12408.
8. D. Lawrence, K. J. Hancock, and S. Kisely, “The Gap in Life Expectancy From Preventable Physical Illness in Psychiatric Patients in Western Australia: Retrospective Analysis of Population Based Registers,” BMJ 346 (2013): f2539, https://doi.org/10.1136/bmj.f2539.
9. E. R. Walker, R. E. McGee, and B. G. Druss, “Mortality in Mental Disorders and Global Disease Burden Implications: A Systematic Review and Meta-Analysis,” JAMA Psychiatry 72, no. 4 (2015): 334, https://doi. org/10.1001/jamapsychiatry.2014.2502.
10. S. Ali, D. Santomauro, A. J. Ferrari, and F. Charlson, “Excess Mortality in Severe Mental Disorders: A Systematic Review and MetaRegression,” Journal of Psychiatric Research 149 (2022): 97–105, https:// doi.org/10.1016/j.jpsychires.2022.02.036.
11. G. Thornicroft, “Physical Health Disparities and Mental Illness: The Scandal of Premature Mortality,” British Journal of Psychiatry 199, no. 6 (2011): 441–442, https://doi.org/10.1192/bjp.bp.111.092718.
12. L. E. Ross, S. Vigod, J. Wishart, et al., “Barriers and Facilitators to Primary Care for People With Mental Health and/or Substance Use Issues: A Qualitative Study,” BMC Family Practice 16, no. 1 (2015): 135, https://doi.org/10.1186/s12875-015-0353-3.
13. B. Happell, D. Scott, and C. Platania-Phung, “Perceptions of Barriers to Physical Health Care for People With Serious Mental Illness: A Review of the International Literature,” Issues in Mental Health Nursing 33, no. 11 (2012): 752–761, https://doi.org/10.3109/01612840.2012. 708099.
14. L. M. Isbell, H. Chimowitz, N. R. Huff, G. Liu, E. Kimball, and E. Boudreaux, “A Qualitative Study of Emergency Physicians' and Nurses' Experiences Caring for Patients WWith Psychiatric Conditions and/or Substance Use Disorders,” Annals of Emergency Medicine January 2023: 81, no. 6 (2023): S0196064422011970, https://doi.org/10.1016/j.annem ergmed.2022.10.014.
15. A. Ronaldson, L. Elton, S. Jayakumar, A. Jieman, K. Halvorsrud, and K. Bhui, “Severe Mental Illness and Health Service Utilisation for Nonpsychiatric Medical Disorders: A Systematic Review and MetaAnalysis,” PLoS Medicine 17, no. 9 (2020): 1–34, https://doi.org/10.1371/ journal.pmed.1003284.
16. L. Santo, “Emergency Department Visits Among Adults With Mental Health Disorders: United States, 2017–2019,” NCHS Data Brief, no. 426 (2021): 1–8.
17. K. Nordstrom, J. Berlin, S. Nash, S. Shah, N. Schmelzer, and L. Worley, “Boarding of Mentally Ill Patients in Emergency Departments: American Psychiatric Association Resource Document,” Western Journal of Emergency Medicine 20, no. 5 (2019): 690–695, https://doi.org/10.5811/westjem.2019.6.42422.
18. B. Armoon, G. Grenier, Z. Cao, C. Huỳnh, and M. J. Fleury, “Frequencies of Emergency Department Use and Hospitalization Comparing 14756773, 0, Downloaded from https://onlinelibrary.wiley.com/doi/10.1111/1475-6773.14617 by Yale University, Wiley Online Library on [21/05/2025]. See the Terms and Conditions (https://onlinelibrary.wiley.com/terms-and-conditions) on Wiley Online Library for rules of use; OA articles are governed by the applicable Creative Commons License 12 of 13 Health Services Research, 2025 Patients With Different Types of Substance or Polysubstance-Related Disorders,” Substance Abuse Treatment, Prevention, and Policy 16, no. 1 (2021): 89, https://doi.org/10.1186/s13011-021-00421-7.
19. D. Lewer, J. Freer, E. King, et al., “Frequency of Health-Care Utilization by Adults Who Use Illicit Drugs: A Systematic Review and MetaAnalysis,” Addiction 115, no. 6 (2020): 1011–1023, https://doi.org/10. 1111/add.14892.
20. P. Croskerry, “ED Cognition: Any Decision by Anyone at any Time,” Canadian Journal of Emergency Medicine 16, no. 1 (2014): 13–19, https:// doi.org/10.2310/8000.2013.131053.
21. L. M. Isbell, E. D. Boudreaux, H. Chimowitz, G. Liu, E. Cyr, and E. Kimball, “What Do Emergency Department Physicians and Nurses Feel? A Qualitative Study of Emotions, Triggers, Regulation Strategi
22. J. A. Giandinoto and K. Leigh Edward, “Challenges in Acute Care of People With Co-Morbid Mental Illness,” British Journal of Nursing 23, no. 13 (2014): 728–732, https://doi.org/10.12968/bjon.2014.23.13.728.
23. J. M. Smith, S. Knaak, J. Smith, et al., “An Exploration of Mental Health-Related Stigma in an Emergency Setting,” International Journal of Mental Health and Addiction (2024): 1–23, https://doi.org/10.1007/ s11469-023-01233-5.
24. S. Jones, L. Howard, and G. Thornicroft, “‘Diagnostic Overshadowing’: Worse Physical Health Care for People With Mental Illness,” Acta Psychiatrica Scandinavica 118, no. 3 (2008): 169–171, https://doi.org/10. 1111/j.1600-0447.2008.01211.x.
25. R. Molloy, G. Brand, I. Munro, and N. Pope, “Seeing the Complete Picture: A Systematic Review of Mental Health Consumer and Health Professional Experiences of Diagnostic Overshadowing,” Journal of Clinical Nursing 32, no. 9–10 (2023): 1662–1673, https://doi.org/10.1111/ jocn.16151.
26. R. Cunningham, F. Imlach, H. Lockett, et al., “Do Patients With Mental Health and Substance Use Conditions Experience Discrimination and Diagnostic Overshadowing in Primary Care in Aotearoa New Zealand? Results From a National Online Survey,” Journal of Primary Health Care 15, no. 2 (2023): 112–121, https://doi.org/10.1071/HC23015.
