
BPD and Suicide Risk
The goal of this work is to clarify the role of the kappa opioid receptor (KOR) in the pathophysiology of borderline personality disorder (BPD), a condition associated with alarmingly high rates of comorbidity and mortality [1-3], but few effective pharmacological interventions [4-5]. Critically, BPD is associated with 75% lifetime suicide attempt (SA) [6] and at least 10% suicide mortality [7] (50x general population) [8]. BPD is characterized by emotion dysregulation, altered pain perception, impulsivity, and self-injurious behavior (SIB) [9-11]. Despite the complexity and seriousness of the disorder, available agents largely fall short of affecting overall symptom severity [12-14] and affecting suicide risk [15-16].
Understanding the pathophysiology of BPD to better inform development of potentially life-saving interventions for this high-risk population must be prioritized.
Growing evidence has implicated the opioid system, and specifically KOR, in the pathophysiology of BPD. The opioid system is instrumental in the regulation of core features of BPD including emotional lability [17], social functioning [18], and the experience of pain [19]. By contrast, KOR has recently received attention as a promising alternative target for intervention in BPD and other stress-related disorders [20], which suggest KOR signaling affects the effect of stress on the development of psychiatric symptoms. Elevated dynorphin (the opioid peptide associated with KOR), which can result from chronic stress [21-22], and activation of KOR are both associated with symptoms of BPD (e.g., dissociation [23], cognitive dysfunction [21]).
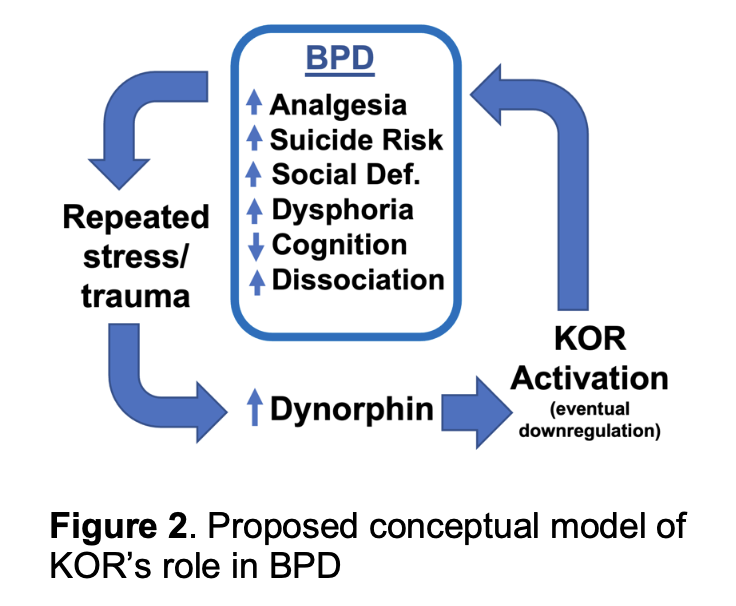
Thus, there is strong support for KOR as a potential treatment target in BPD. However, the role and clinical relevance of KOR in BPD, including potential sex differences, is not yet well understood.
With novel radiotracer [11C]EKAP, we can now reliably quantify KOR availability in vivo with positron emission tomography (PET).
Our goals:
Determine whether BPD and a history of suicide attempt (SA) are associated with dysregulation in KOR availability
Examine the association between KOR availability and other correlates of BPD and suicide risk – impulsivity, emotion regulation, and symptom severity.
Examine sex differences in the association between KOR availability and BPD.
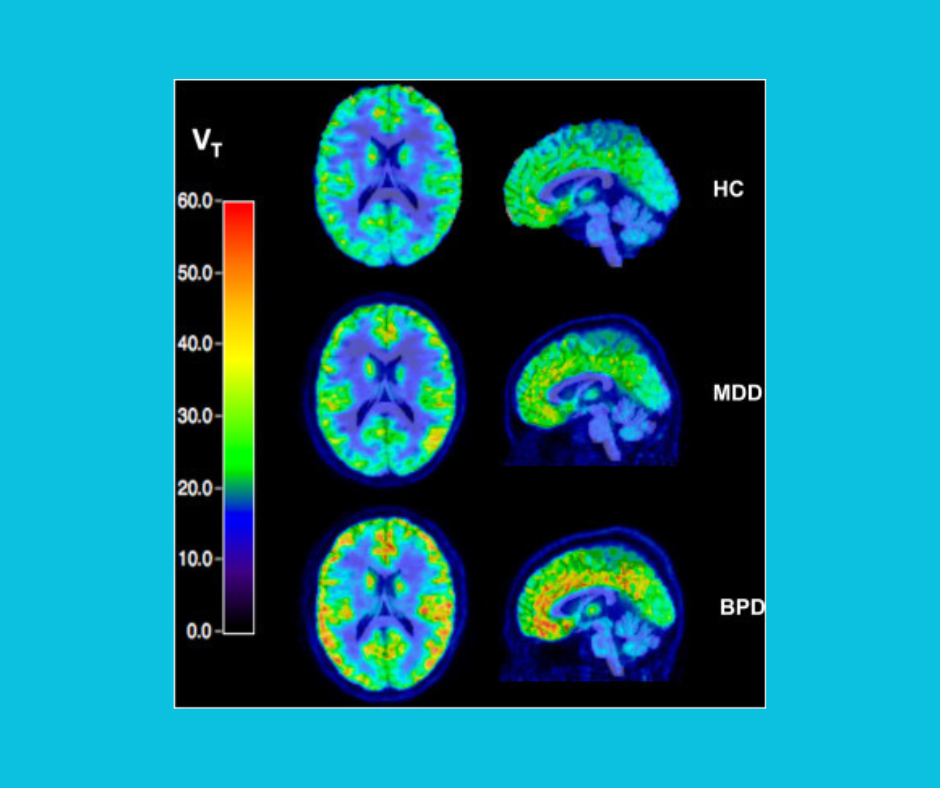
Image displaying the relationship between mGlu5 availability and suicide ideation
Suggested reading:
Resources
Citations
Bolton JM, Pagura J, Enns MW, Grant B, Sareen J. A population-based longitudinal study of risk factors for suicide attempts in major depressive disorder. J Psychiatr Res. 2010;44(13):817-826.
Soloff PH, Lynch KG, Kelly TM, Malone KM, Mann JJ. Characteristics of suicide attempts of patients with major depressive episode and borderline personality disorder: a comparative study. American Journal of Psychiatry. 2000;157(4):601-608.
Stringer B, van Meijel B, Eikelenboom M, Koekkoek B, Licht CM, Kerkhof AJ, Penninx BW, Beekman AT. Recurrent suicide attempts in patients with depressive and anxiety disorders: the role of borderline personality traits. Journal of affective disorders. 2013;151(1):23-30.
Ripoll LH. Psychopharmacologic treatment of borderline personality disorder. Dialogues in clinical neuroscience. 2013;15(2):213.
Ripoll LH. Clinical psychopharmacology of borderline personality disorder: an update on the available evidence in light of the Diagnostic and Statistical Manual of Mental Disorders–5. Current opinion in psychiatry. 2012;25(1):52-58.
Paris J, Zweig-Frank H. A 27-year follow-up of patients with borderline personality disorder. Comprehensive psychiatry. 2001;42(6):482-487.
Black DW, Blum N, Pfohl B, Hale N. Suicidal behavior in borderline personality disorder: prevalence, risk factors, prediction, and prevention. Journal of personality disorders. 2004;18(3: Special issue):226-239.
Skodol AE, Gunderson JG, Pfohl B, Widiger TA, Livesley WJ, Siever LJ. The borderline diagnosis I: psychopathology, comorbidity, and personaltity structure. Biological psychiatry. 2002;51(12):936-950.
Klonsky ED, May A. Rethinking impulsivity in suicide. Suicide and Life-Threatening Behavior. 2010;40(6):612-619.
Van Orden KA, Witte TK, Cukrowicz KC, Braithwaite SR, Selby EA, Joiner Jr TE. The interpersonal theory of suicide. Psychological review. 2010;117(2):575.
Mann JJ, Arango VA, Avenevoli S, Brent DA, Champagne FA, Clayton P, Currier D, Dougherty DM, Haghighi F, Hodge SE. Candidate endophenotypes for genetic studies of suicidal behavior. Biological psychiatry. 2009;65(7):556-563.
Lieb K, Völlm B, Rücker G, Timmer A, Stoffers JM. Pharmacotherapy for borderline personality disorder: Cochrane systematic review of randomised trials. The British Journal of Psychiatry. 2010;196(1):4-12.
Ingenhoven T, Lafay P, Rinne T, Passchier J, Duivenvoorden H. Effectiveness of pharmacotherapy for severe personality disorders: meta-analyses of randomized controlled trials. 2010.
Ingenhoven TJ, Duivenvoorden HJ. Differential effectiveness of antipsychotics in borderline personality disorder: meta-analyses of placebo-controlled, randomized clinical trials on symptomatic outcome domains. Journal of clinical psychopharmacology. 2011;31(4):489-496.
Lutz PE, Courtet P, Calati R. The opioid system and the social brain: implications for depression and suicide. Journal of neuroscience research. 2018.
Hancock-Johnson E, Griffiths C, Picchioni M. A Focused Systematic Review of Pharmacological Treatment for Borderline Personality Disorder. CNS drugs. 2017;5(31):345-356.
New AS, Stanley B. An opioid deficit in borderline personality disorder: self-cutting, substance abuse,
and social dysfunction: Am Psychiatric Assoc; 2010.
Kennedy SE, Koeppe RA, Young EA, Zubieta J-K. Dysregulation of endogenous opioid emotion
regulation circuitry in major depression in women. Archives of general psychiatry. 2006;63(11):1199-
Chavkin C. The therapeutic potential of κ-opioids for treatment of pain and addiction. Neuropsychopharmacology. 2011;36(1):369.
Jacobson ML, Browne CA, Lucki I. Kappa opioid receptor antagonists as potential therapeutics for
stress-related disorders. Annual review of pharmacology and toxicology. 2020;60:615-636.
Bruchas M, Land B, Chavkin C. The dynorphin/kappa opioid system as a modulator of stress-induced
and pro-addictive behaviors. Brain research. 2010;1314:44-55.
Smith JS, Schindler AG, Martinelli E, Gustin RM, Bruchas MR, Chavkin C. Stress-induced activation of
the dynorphin/κ-opioid receptor system in the amygdala potentiates nicotine conditioned place
preference. Journal of Neuroscience. 2012;32(4):1488-1495.
MacLean KA, Johnson MW, Reissig CJ, Prisinzano TE, Griffiths RR. Dose-related effects of salvinorin
A in humans: dissociative, hallucinogenic, and memory effects. Psychopharmacology.
2013;226(2):381-392.
This study is possible due to support from NIMH.

